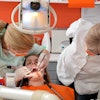
SAN FRANCISCO - California should change restrictive licensing regulations, reinstate the Denti-Cal program for adults, and appoint a state dental director to improve oral health services for underserved populations, according to oral care experts who met August 4 to discuss barriers to access to care.
Academics and public health officials joined representatives from U.S. government programs and professional dental groups to discuss ways to overcome barriers to access to care for underserved Californians. The panelists were members of the Committee on Oral Health Access to Services, which wrote the Institute of Medicine's (IOM) 234-page report, "Improving Access to Oral Health Care for Vulnerable and Underserved Populations," released in July. The workshop was held in conjunction with the California HealthCare Foundation, a co-sponsor of the report.
Among other things, that report authors found that millions of Americans are not receiving needed dental care services because of "persistent and systemic" barriers that limit their access to oral healthcare.
In California, restrictive licensing regulations should to be changed so that dental students and dental assistants can provide more services to the poor in community health centers, according to several panelists at the meeting.
William Bird, DDS, MPH, DrPH, a professor at the University of California, San Francisco, (UCSF) School of Dentistry, said licensing requirements are keeping oral care providers from using their training to help underserved populations.
"They can't bill for things they're not licensed for," he said, adding that billing procedures also need to be revised.
Dental students working at federally qualified health centers (FQHCs) cannot get Medicaid reimbursements because of licensing requirements, noted Robert Isman, DDS, MPH, a dental program consultant with the California Department of Health Care Services' Medi-Cal Dental Services.
Registered dental assistants (RDA) are no longer allowed to do dental screenings in public health settings due to a new interpretation of the law by the Dental Board of California, said Margaret Fisher, RDHAP, a consultant in the Children's Health and Disability Prevention Program in the San Francisco Department of Public Health. About 30% of the preschool children that she sees have visible caries, she said.
“There are workforce, regulatory, and reimbursement barriers.”
— Paul Glassman, DDS, University of the
Pacific Arthur A. Dugoni School of
Dentistry
Also, exemptions should be made to allow dental professionals working for FQHCs to provide services outside their facilities, at locations such as schools and community centers, said Jim Stephens, DDS, a Palo Alto dentist who is secretary of the CDA.
Nationwide budget deficits have caused many states to cut their Medicaid programs and reimbursement rates, with adult dental benefits being one of the hardest hit sectors.
Some 40% of Californians are uninsured, according to Elizabeth Mertz, PhD, an assistant professor at the UCSF School of Dentistry. The state's Denti-Cal program for adults was cut in 2009, Mertz said, and California has some of the lowest Medicaid reimbursement rates in the country.
With the ongoing wrangling in Washington, DC, over the federal debt, California could see the $1 billion the state was slated to receive as part of the Affordable Care Act drastically reduced. The money was supposed to be used to fund FQHCs, scholarships, and loan repayment programs for medical professionals, including dentists, said Tahira Bazile, the associate director of policy for the California Primary Care Association (CPCA), the trade group for nonprofit clinics.
Federal officials already have announced that $600 million will be cut from the $11 billion that was slated to support and expand FQHCs nationwide during the next five years, Bazile said.
Now, only six or seven new FQHCs will be built in California instead of the 40 to 50 that were planned before the cuts, she said.
Midlevel providers debated
The issue of midlevel providers is referred to in the IOM report as a possible, albeit "controversial," solution to the access-to-care issue that needs more research to determine how they would be reimbursed and licensed. The concept generated some of the most heated discussions at the San Francisco meeting.
Lisa Okamoto, RDH, president of the California Dental Hygienists' Association -- which supports the midlevel provider concept -- referred to the issue as "that dirty word," a reference to the opposition by a majority of professional dental groups in the U.S.
It is a complicated issue involving several factors, according to Paul Glassman, DDS, a professor and the director of community oral health at the University of the Pacific Arthur A. Dugoni School of Dentistry.
"There are workforce, regulatory, and reimbursement barriers, and if we were to try to solve the problem with only one of those -- just the workforce solution -- it wouldn't achieve what we want, which is to get care to the underserved population," Dr. Glassman told DrBicuspid.com, noting that he was speaking on a personal level, not as an IOM committee member. "If we can be successful at creating a regulatory and reimbursement environment where people can actually see underserved populations using multiple strategies, then we can begin to intelligently think about what is the new workforce that we need."
Midlevel providers have been used in more than 40 countries for nearly a century and are part of public health systems that receive government support in those countries, Dr. Glassman added.
Dr. Bird, who served for 24 years in the U.S. Public Health Service's Indian Health Service, called midlevel providers a "hot button" issue. Even so, he told DrBicuspid.com, "I think they have a role."
The CPCA also supports the new workforce model, Bazile said.
Dr. Stephens of the CDA said there is insufficient research regarding the safety of allowing nondentists to perform irreversible procedures. And James Thompson, DMD, a San Diego dentist who is a trustee of the Academy of General Dentistry, derided the concept as "second-class care" from a two-tiered healthcare system that is "economically unfeasible."
Several panelists also called for the reappointment of a state dental director, saying it would help with California's dental advocacy efforts in Sacramento and Washington, DC.